

|
PTSD:
|
A continuing education course for 12 ces
consisting
of reading and taking a post-test on:

 |
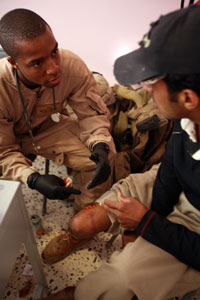
| Establishing Therapeutic Alliance Many people with PTSD find that their relationships with others have changed as a result of exposure to trauma. They often report that they have difficulty trusting others, are suspicious of authority, dislike even minor annoyances, and generally want to be left alone. Since the clinician-patient relationship draws heavily on trust, respect, and openness, and since the relationship often has to be formed in a busy clinical or bureaucratic setting, the provider may find the PTSD patient to seem to be withholding, negativistic, or even hostile at the initial meeting. The patient may seem to have “an attitude,” or “Axis II” co-morbidity. As a result, many combat veterans feel misunderstood or misdiagnosed by otherwise competent professionals, and ultimately the patient suffers through feeling betrayed and misunderstood by the mental health professional. If a therapeutic relationship is to have any opportunity to develop, the treatment provider must adopt a stance of caring and concerned involvement that takes what the patient says at face value, doesn’t judge or label this type of behavior, and doesn’t withdraw into an “objective” “professional” role. In short, the clinician who can relate honestly and openly is more likely to have a patient who is willing to relate to him/her as a fellow human being and an effective partner in treatment. A general understanding of what has happened to the veteran is critical in this process of developing a therapeutic relationship. Every provider working with combat veterans should be advised to read some basic material on the experience of combat and watch documentaries of the same. The provider must develop an understanding that wartime and military service involves some of the most intense human experiences and that those feelings of profound rage, fear, and grief can be an expected part of these experiences. These feelings will be present in the interview setting and must be met with respect and compassion. It is also helpful for the professional to be careful not to assume that they have any understanding of the military experience if they have not themselves served in the military and should not be afraid to ask questions when they don’t understand something about the military that the patient is referring to. Family, religious organizations and community leaders can be helpful when dealing with an unfamiliar culture and/or religion. It may also be appropriate to consult a local cultural adviser. But particular attention should be paid to the individual’s own beliefs and values, and confidentiality always must be maintained when getting input from other sources. Patient’s beliefs should be seen in the context of their social, religious, and cultural environment, and if need be, a trusted member of the person’s faith or cultural group should be consulted. |
| RECOMMENDATIONS Treatment Options: 1. Strongly recommend that patients who are diagnosed with PTSD should be offered one of the evidence-based trauma-focused psychotherapeutic interventions that include components of exposure and/or cognitive restructuring; or stress inoculation training. [A] The choice of a specific approach should be based on the severity of the symptoms, clinician expertise in one or more of these treatment methods and patient preference, and may include an exposure-based therapy (e.g., Prolonged Exposure), a cognitive-based therapy (e.g., Cognitive Processing Therapy), Stress management therapy (e.g., SIT) or Eye Movement Desensitization and Reprocessing (EMDR). 2. Relaxation techniques should be considered as a component of treatment approaches for ASD or PTSD in alleviating symptoms associated with physiological hyper-reactivity. [C] 3. Imagery Rehearsal Therapy [IRT] can be considered for treatment of nightmares and sleep disruption. [C] 4. Brief Psychodynamic Therapy can be considered for patients with PTSD. [C] 5. Hypnotic Techniques can be considered, especially for symptoms associated with PTSD, such as pain, anxiety, dissociation, and nightmares, for which hypnosis has been successfully used. [C] 6. There is insufficient evidence to recommend for or against Dialectical Behavioral Therapy (DBT) as first-line treatment for PTSD [I] • Dialectical Behavioral Therapy can be considered for patients with a borderline personality disorder typified by parasuicidal behaviors. [B] 7. There is insufficient evidence to recommend for or against Family or Couples Therapy as first-line treatment for PTSD; Family or Couples therapy may be considered in managing PTSD-related family disruption or conflict, increasing support, or improving communication. [I] 8. Group Therapy may be considered for treatment of PTSD [C] • There is insufficient evidence to favor any particular type of group therapy over other types • Patients being considered for group therapy should exhibit acceptance for the rationale for trauma work, and willingness to self-disclose in a group. 9. Consider augmenting with other effective evidence-based interventions for patients who do not respond to a single approach. 10.Supportive psychotherapy is not considered to be effective for the treatment of PTSD. However, multiple studies have shown that supportive interventions are significantly more helpful than no treatment, and they may be helpful in preventing relapse in patients who have reasonable control over their symptoms and are not in severe and acute distress. Note: Approaches may also be beneficial as parts of an effectively integrated approach. Most experienced therapists integrate diverse therapies, which are not mutually exclusive, in a fashion that is designed to be especially beneficial to a given patient. |

TABLE OF CONTENTS INTRODUCTION 4 |
maintains responsibility for the program. |
|
The Clinician will be able to: 1. Triage and manage acute traumatic stress
|
Assess Pre-Existing Psychiatric and Medical Conditions Risk Factors for ASD |
To read the course material without receiving credit or taking a post-test, go now to: VA/DoD CLINICAL PRACTICE GUIDELINE FOR MANAGEMENT OF POST-TRAUMATIC STRESS You
will need Adobe Acrobat in order to read this. Adobe Acrobat is certified virus free |
We do adhere to the American Psychological Association's Ethical Principles of Psychologists. Our courses are carefully screened by the Planning Committee to adhere to APA standards. We also require authors who compose Internet courses specifically for us follow APA ethical standards. Many of our courses contain case material, and may use the methods of qualitative research and analysis, in-depth interviews and ethnographic studies. The psychotherapeutic techniques depicted may include play therapy, sandplay therapy, dream analysis, drawing analysis, client and therapist self-report, etc. The materials presented may be considered non-traditional and may be controversial, and may not have widespread endorsement within the profession. www.psychceu.com maintains responsibility for the program and its content. |
All material included in this course is either in the public domain, or used with express permission. |
Cost of the 12 unit course is $143
![]()